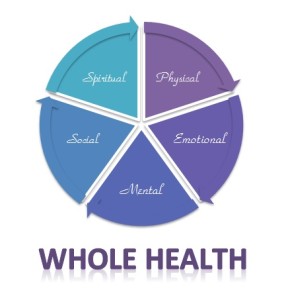
 Women currently have a spectrum of childbirth options ranging between unassisted natural homebirth, and elective cesarean section. Somewhere between those two extremes lies two models of care generally referred to as the “midwifery model”, and the “medical model”. These models have been analyzed time and time again, but the controversy about which is preferable has not lessened. This may be because the models have primarily been evaluated in only one area of health, Physical Health, and in that one area they are arguably equal. However, to fairly compare the benefits of the two models it is vital to evaluate them in context of Whole Health, which is made up of five parts: Physical Health, Emotional Health, Mental Health, Social Health, and Spiritual Health. When compared this way, in the arena of Whole Health, it becomes clear that the midwifery model offers much more than the medical model.
Women currently have a spectrum of childbirth options ranging between unassisted natural homebirth, and elective cesarean section. Somewhere between those two extremes lies two models of care generally referred to as the “midwifery model”, and the “medical model”. These models have been analyzed time and time again, but the controversy about which is preferable has not lessened. This may be because the models have primarily been evaluated in only one area of health, Physical Health, and in that one area they are arguably equal. However, to fairly compare the benefits of the two models it is vital to evaluate them in context of Whole Health, which is made up of five parts: Physical Health, Emotional Health, Mental Health, Social Health, and Spiritual Health. When compared this way, in the arena of Whole Health, it becomes clear that the midwifery model offers much more than the medical model.
The first area of health is Physical Health – wellness of our physical body. The threats to a woman’s physical health during pregnancy and childbirth are the main focus of the medical model of childbirth. Medical model practitioners routinely examine and evaluate for any signs of disease or distress at prenatal visits, undermining the idea that a woman’s body is capable of carrying her baby successfully. During the birth, a woman labors under an expectant cloud of potential labor failures, and is actually subjected to physical harm; by injection, restraint, starvation, etc…; under the premise that she will be more ready for intervention in the inevitable case of emergency. The midwifery model practitioner, in contrast, begins the pregnancy by verifying signs of normalcy and reassuring a woman of her body’s ability to carry her baby to term. Each prenatal visit, the normalcy is reaffirmed, encouraging a woman to have faith in her body. During labor, a woman participating in midwifery care will not be needlessly harmed, but will be supported to work with her body in an atmosphere where the expectation is that “normal” will proceed as usual. A midwife is not unprepared for emergency, though. The midwifery model demands the ability of the midwife to perform all lifesaving skills in nearly identical ways to those found in a hospital birthing suite. In the area of Physical Health, both models do a good job ensuring the outcome of a live mother and baby, with only very slight (and highly arguable) differences in mortality and morbidity rates.
The second area of health is Emotional Health – respecting and managing emotions. This area shows even more contrast between the two models of care. Emotional health is largely ignored in medical model, with the focus almost solely on the physical aspect of childbirth. Negative emotional issues are viewed as personal or even dysfunctional, but not significant to the birth process. A medical model practitioner may be sympathetic to a woman’s emotional turmoil, but rarely connects those emotions to possible issues during pregnancy and childbirth. During pregnancy the emotionally significant “first-time” moments are often lost in the rush of the 15 minute appointment. At birth, a mother and her family are generally left alone to deal with the emotional turbulence of labor while the medical practitioners watch machines, often in different rooms, to determine the status of the patient. After the birth, the important emotional bonding between mother and baby is interrupted by unnecessary intervention and separation. The MMC, conversely, views the importance of emotional health during pregnancy and childbirth as being on nearly equal ground with physical health. During pregnancy, a midwife is aware of the importance of each emotional milestone, and takes care to allow plenty of time for each woman and family to fully experience the wonder of her growing baby. At birth, a midwife is with a woman to help her navigate the emotional ups and downs of labor, and will recognize negative emotional issues as possible hindrances to progress. A MMC practitioner is trained to address these issues to help a woman to move past them and birth her baby successfully. After the birth a midwife is willing to put off any unneeded interventions until the mother, baby, and family have been able to bask in the amazing splendor of the moment. Clearly, the MMC does a better job of caring for a woman’s emotional health.
largely ignored in medical model, with the focus almost solely on the physical aspect of childbirth. Negative emotional issues are viewed as personal or even dysfunctional, but not significant to the birth process. A medical model practitioner may be sympathetic to a woman’s emotional turmoil, but rarely connects those emotions to possible issues during pregnancy and childbirth. During pregnancy the emotionally significant “first-time” moments are often lost in the rush of the 15 minute appointment. At birth, a mother and her family are generally left alone to deal with the emotional turbulence of labor while the medical practitioners watch machines, often in different rooms, to determine the status of the patient. After the birth, the important emotional bonding between mother and baby is interrupted by unnecessary intervention and separation. The MMC, conversely, views the importance of emotional health during pregnancy and childbirth as being on nearly equal ground with physical health. During pregnancy, a midwife is aware of the importance of each emotional milestone, and takes care to allow plenty of time for each woman and family to fully experience the wonder of her growing baby. At birth, a midwife is with a woman to help her navigate the emotional ups and downs of labor, and will recognize negative emotional issues as possible hindrances to progress. A MMC practitioner is trained to address these issues to help a woman to move past them and birth her baby successfully. After the birth a midwife is willing to put off any unneeded interventions until the mother, baby, and family have been able to bask in the amazing splendor of the moment. Clearly, the MMC does a better job of caring for a woman’s emotional health.
 The third area of health is Mental Health – learning, enabling personal ability, and problem solving. The MdM does not place an emphasis on enriching a woman’s mental health, preferring instead to deliver neatly censored bits of information designed to guide a woman down a prescribed path. Unpopular options may be presented with extreme bias, and alternative views are largely ignored. Some practitioners even prefer that a woman does not attempt to learn about her pregnancy and birth so that she does not question, or attempt to interfere with the routine protocols. This is very different in the MMC, which encourages women to explore all possibilities and become truly educated about their options. Midwives often have an extensive, diverse learning library that includes everything from medical texts to writings from the extreme fringe. In the MMC, women are expected to make educated decisions about their own care. Midwives are generally very supportive of a woman’s personal choices because they know that education and empowerment are important pieces of a successful birth. This knowledge makes MMC a better choice for women interested in enriching their mental health.
The third area of health is Mental Health – learning, enabling personal ability, and problem solving. The MdM does not place an emphasis on enriching a woman’s mental health, preferring instead to deliver neatly censored bits of information designed to guide a woman down a prescribed path. Unpopular options may be presented with extreme bias, and alternative views are largely ignored. Some practitioners even prefer that a woman does not attempt to learn about her pregnancy and birth so that she does not question, or attempt to interfere with the routine protocols. This is very different in the MMC, which encourages women to explore all possibilities and become truly educated about their options. Midwives often have an extensive, diverse learning library that includes everything from medical texts to writings from the extreme fringe. In the MMC, women are expected to make educated decisions about their own care. Midwives are generally very supportive of a woman’s personal choices because they know that education and empowerment are important pieces of a successful birth. This knowledge makes MMC a better choice for women interested in enriching their mental health.
Next there is Social Health – learning how to communicate, building confidence in and trust in one’s self. The MdM can be socially challenging because medical providers can easily speak over a woman’s head, or rely mostly on monitors to assess a patient’s progress. This can leave a void in a woman’s social center, and she might feel removed or unimportant in the social sphere of her own care. This is poignantly demonstrated in the pushing stage of labor where, in the MdM, a woman is told by her provider when she should, or should not push, and encouraged to ignore her own instinct. In the MMC, the pregnant woman is the social center of care. She is relied on to convey her feelings, and sense of progress. She is the director of her own pushing stage, and is not ignored over machines. The MMC supports a woman’s to communicate and trust in herself, making it the preferable choice for social wellness.
The last area of health to be examined is Spiritual Health – exploring a relationship with the divine, and discovering a sense of greater purpose. Spiritually, the MdM is silent. Childbirth is viewed as a clinical routine; and undertaking of technical nature. No mention of the powerful spiritual transition to motherhood can be found in a medical textbook, and there is no acknowledgement of the importance of the “rite of passage” that occurs during a natural labor. In the MMC, however, pregnancy and childbirth are embraced as the deeply spiritual events that they are, and a woman is encouraged to communicate with her divinity in order to bring about the changes in her mind, body, and spirit that need to happen for a successful transition into motherhood. Midwives understand that labor is not incidental, but is am important transition for a woman’s spiritual self. The MMC teaches midwives to help guide a woman on this spiritual journey, making it the superior choice in the Spiritual Health arena.
In summary, it is well known that our general wellbeing does not consist of only our physical health, but requires that all areas of health be nurtured and balanced. While both the MdM and MMC provide excellent care in regard to the physical wellbeing of the mother and baby, the MMC clearly provides superior care for the whole person, and addresses all areas of wellness. This focus on the whole person makes the MMC the best choice for women with uncomplicated pregnancies.